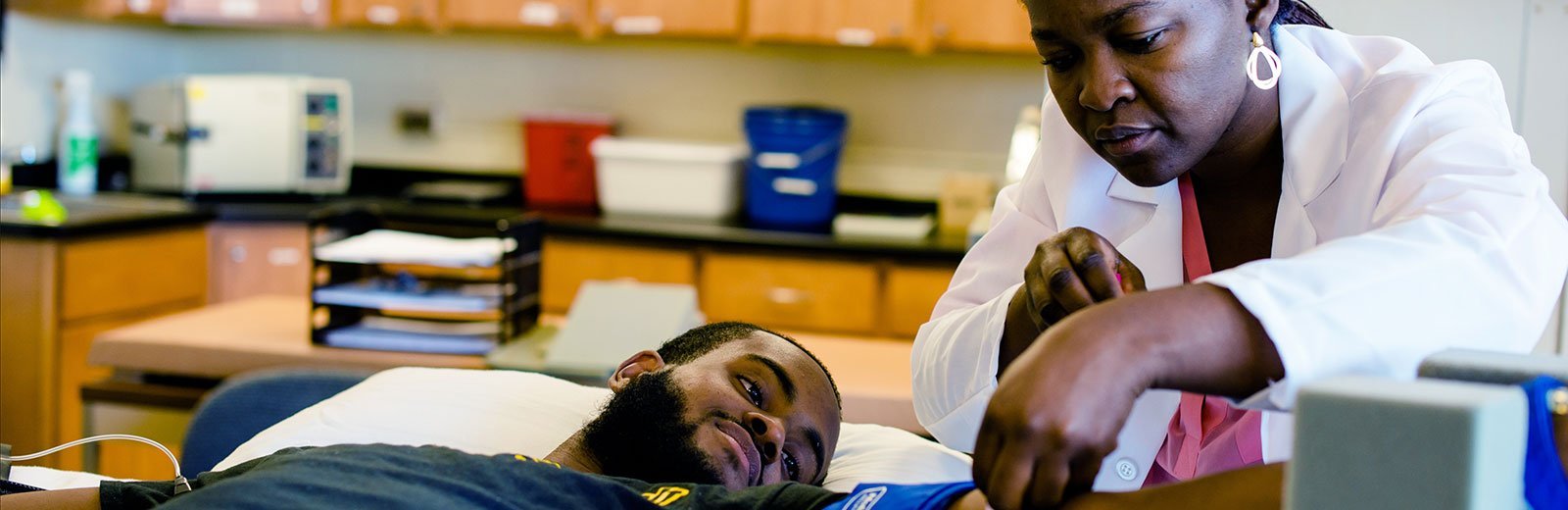
Ida Fonkoue started her medical career in Cameroon, where she grew up, and practiced briefly as a physician. Now a doctoral student at Michigan Tech, Fonkoue swapped the clinic for the research lab.

In the Department of Kinesiology and Integrated Physiology, she studies the effect of various stressors on the sympathetic nervous system, our built-in fight or flight response.
Fonkoue is humble about her research, calling it "a stone in the ocean," reminding us that science is iterative, exploratory and built stone by stone. But she does have a personal vision for how to revolutionize the way we approach physiology research.
Q: What's the big picture challenge you tackle in your research?
A: As an African-American, I belong to a group with a high prevalence of hypertension [high blood pressure] according to the American Heart Association heart and stroke statistics. Alcohol is known to stimulate the sympathetic nervous system and therefore raise blood pressure. My dissertation is trying to look at whether or not the interaction between alcohol and race has a significant effect on muscle sympathetic nerve activity.
Broken down: I want to know if African-Americans would have a higher sympathoexcitation induced by alcohol than their Caucasian counterparts. That was the big question I want to answer in my research—and it's always difficult to completely answer a question in one project. But at least that's the door I want to take and then maybe other people in the future can go through with the same thinking.

Q: How do you study sympathoexcitation?
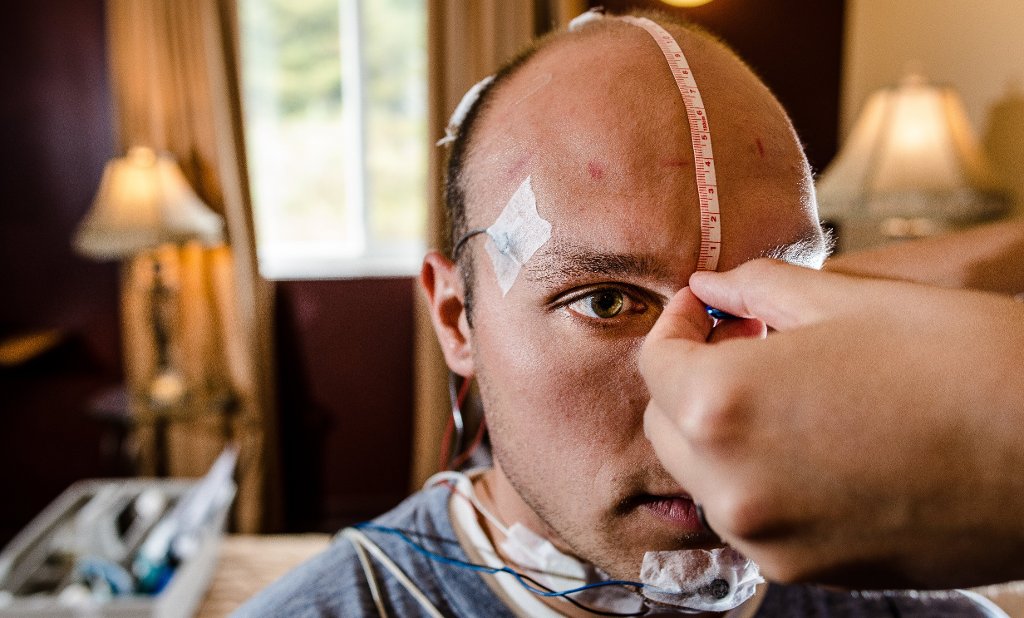
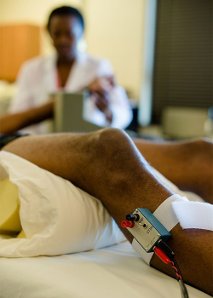
A: Our lab uses a technique called microneurography; to date, it's the gold standard for measuring the activity of post-ganglionic sympathetic nerves. In our case, we're looking at the lower leg. This technique uses a tungsten electrode about the size of an acupuncture needle. One is inserted in the peroneal nerve [below the knee or on the outside of the calf] and it records the signal of post-ganglionic fibers. The signal is amplified afterwards and because the amplifier is connected to a computer, we can see the bursts of activity.
These nerve signal "waves" start in your brain. Imagine then if you have waves in the ocean, at the end of the wave the water is pushing sand away from the beach. You can look at the effect on the sand, which is like measuring adrenaline in the blood, and you can see how strong each wave was and how many waves you had. But what we're doing is analyzing the wave as it's passing by. You can stand somewhere in the way of the waves and you can determine how strong each wave is and how frequently they pass. That's what we do with microneurography.
"I make the case that who we treat should matter as much as what we treat, and that the future of a cost-effective management of hypertension lies in the individualization of treatment. It matters a great deal to be able to understand interindividual physiological differences."Ida Fonkoue
Q: Your microneurography tests note a difference between alcohol's effect on sympathoexcitation in African-Americans and Caucasians. What does that mean for treating hypertension?
A: The treatment of hypertension, depending on how severe it is, often includes or is limited to lifestyle changes. Alcohol intake is often part of those changes, given how it stimulates the sympathetic nervous system. Most tests studying alcohol-blood pressure effects were done on Caucasians. So we knew the general effect of alcohol on blood pressure was mostly true for a given group of individuals, but African-Americans did not seem to respond physiologically as we expected. My research on its own is not sufficient to change medical practices, but it raises questions about generalizing treatment protocols to all people when in fact it applies to some people.
This difference might not all be attributed to race but instead to other environmental factors influencing the sympathetic nervous system and blood pressure in each group.
Q: You call this "individualization" in your work. What does it mean?
A: When we talk about hypertension, it's important for physicians to think about, "Who am I dealing with as much as they think about what? And how does this patient regulate their blood pressure?"
We are used to saying that people are different; it is true physically and even more so physiologically. We now know even more with current research that various factors—environment, obesity, physical activity, kinds of activity, race, sex—all influence people's physiology. Especially when it comes to blood pressure regulation. So in individualizing treatments, we'd be able to deal with each person according to how their system functions; the medication can just help the system work better. And we'll be able to achieve greater results with fewer molecules, in my opinion.
"A wave's effect on sand is like a nerve signal's effect on adrenaline in the blood . . . you can see how strong the waves are by how much the sand is moved."
In Cameroon, people often do not have enough money to get into lifetime treatment, which is usually needed for chronic diseases like hypertension and diabetes. It will be cheaper to find ways to prevent these diseases rather than trying to have people pay for the treatments. And in the event that prevention doesn't work, a better understanding of physiology will allow the right cost effective medical approach to be implemented.
Michigan Technological University is a public research university founded in 1885 in Houghton, Michigan, and is home to more than 7,000 students from 55 countries around the world. Consistently ranked among the best universities in the country for return on investment, Michigan’s flagship technological university offers more than 120 undergraduate and graduate degree programs in science and technology, engineering, computing, forestry, business and economics, health professions, humanities, mathematics, social sciences, and the arts. The rural campus is situated just miles from Lake Superior in Michigan's Upper Peninsula, offering year-round opportunities for outdoor adventure.